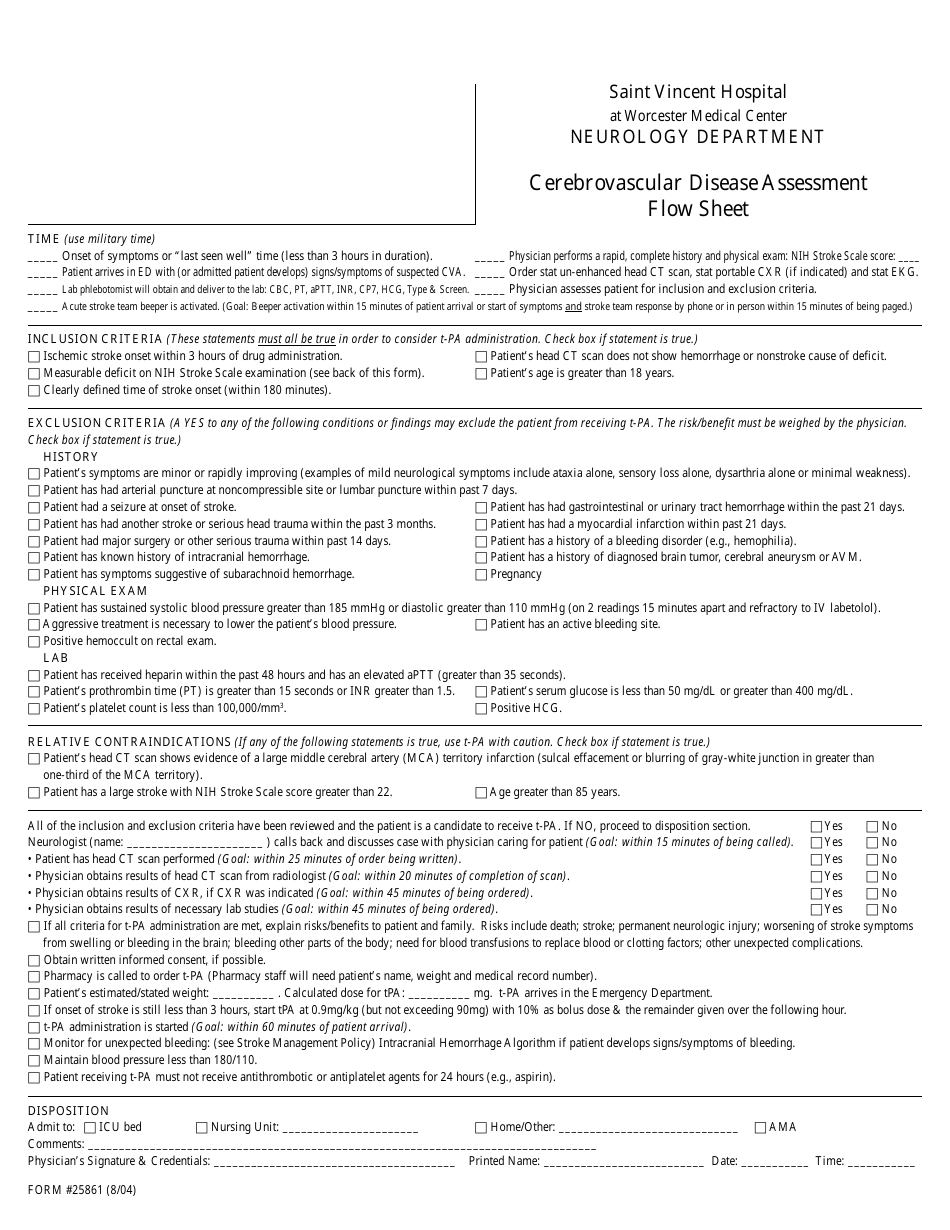
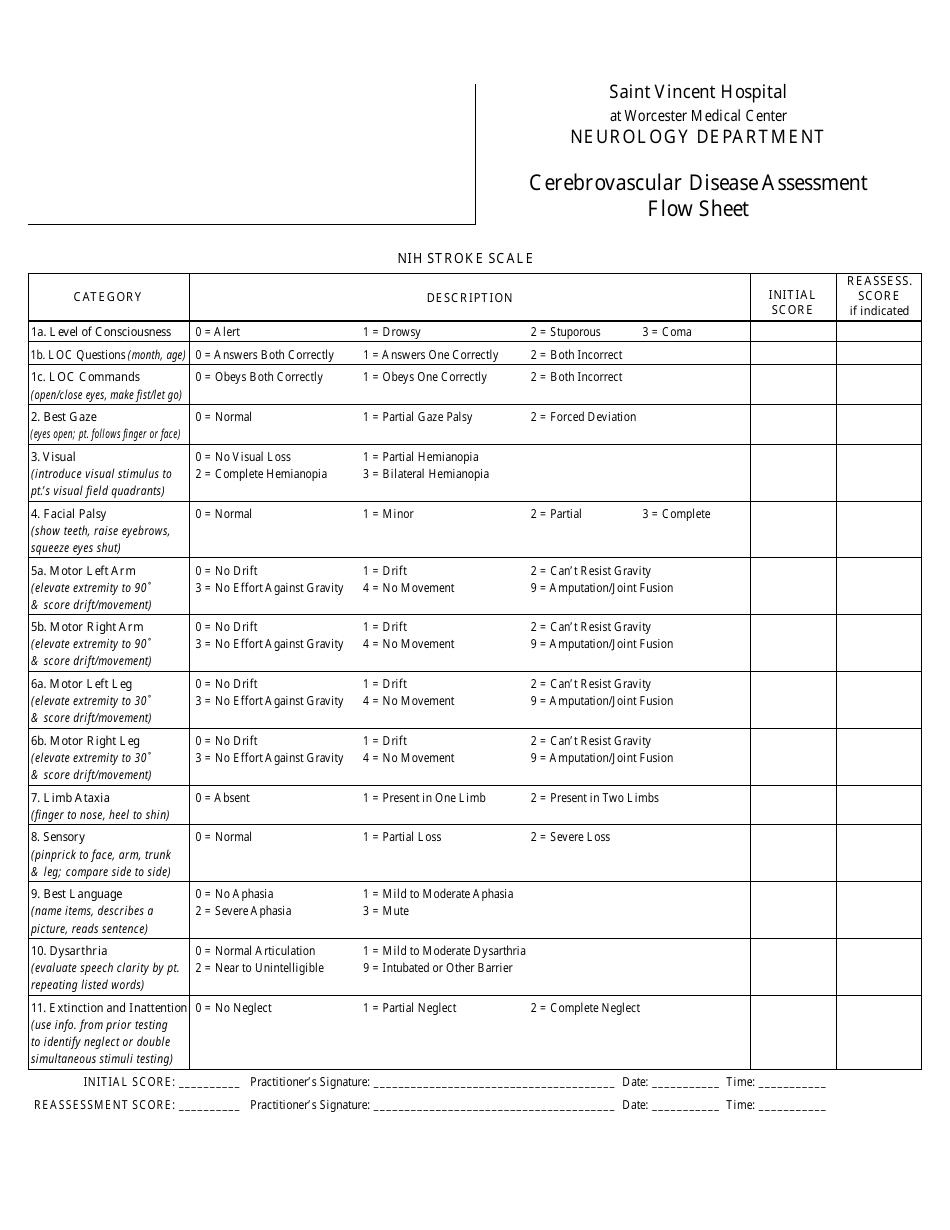
Cerebrovascular Disease Assessment Flow Sheet - Saint Vincent Hospital
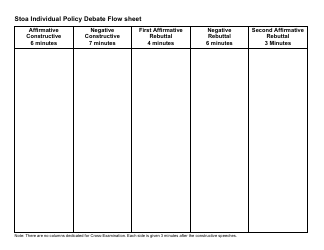
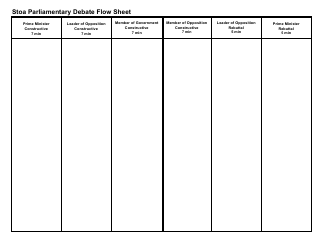
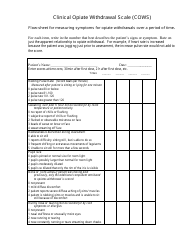
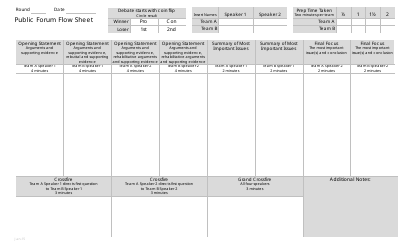
The Cerebrovascular Disease Assessment Flow Sheet at Saint Vincent Hospital is a document used for assessing and monitoring patients who have or are at risk of cerebrovascular disease. It helps healthcare providers track the patient's condition, vital signs, medications, and other important information to provide appropriate care.
FAQ
Q: What is a cerebrovascular disease?
A: Cerebrovascular disease is a condition that affects the blood vessels supplying the brain.
Q: What are the risk factors for cerebrovascular disease?
A: Risk factors for cerebrovascular disease include high blood pressure, smoking, diabetes, high cholesterol, and a family history of the condition.
Q: What are the symptoms of cerebrovascular disease?
A: Symptoms of cerebrovascular disease may include sudden weakness or numbness on one side of the body, difficulty speaking or understanding speech, sudden severe headache, and difficulty with balance or coordination.
Q: How is cerebrovascular disease diagnosed?
A: Cerebrovascular disease can be diagnosed through physical examination, imaging tests such as CT or MRI scans, and blood tests to evaluate risk factors and rule out other conditions.
Q: What are the treatment options for cerebrovascular disease?
A: Treatment options for cerebrovascular disease may include medications to control blood pressure and cholesterol, lifestyle changes such as quitting smoking and adopting a healthy diet, and in some cases, surgical procedures to remove blockages or repair damaged blood vessels.
Q: What can I do to reduce my risk of cerebrovascular disease?
A: To reduce your risk of cerebrovascular disease, it is important to maintain a healthy lifestyle by exercising regularly, eating a balanced diet, avoiding smoking, managing stress, and controlling risk factors such as high blood pressure, diabetes, and high cholesterol.
Q: What should I do if I experience symptoms of cerebrovascular disease?
A: If you experience symptoms of cerebrovascular disease, such as a sudden severe headache, weakness or numbness on one side of the body, or difficulty speaking, it is important to seek immediate medical attention as these symptoms may indicate a stroke.
Q: Can cerebrovascular disease be prevented?
A: While it may not be possible to prevent cerebrovascular disease entirely, you can reduce your risk by making healthy lifestyle choices, managing underlying conditions, and following medical advice to control risk factors.