Suicide Risk Assessment Template
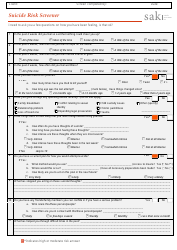
A Suicide Risk Assessment Template is a tool used by mental health professionals to evaluate an individual's risk for suicide. It helps in identifying key factors and warning signs, assessing the severity of suicidal thoughts or behaviors, and determining appropriate interventions or treatment plans. This template helps clinicians systematically gather important information to make informed decisions about a person's safety and support their mental well-being.
The Suicide Risk Assessment Template is typically filled out by mental health professionals, such as psychiatrists, psychologists, or therapists.
FAQ
Q: What is a Suicide Risk Assessment Template?
A: A Suicide Risk Assessment Template is a tool used by mental health professionals to evaluate an individual's risk for suicide.
Q: What does a Suicide Risk Assessment Template include?
A: A Suicide Risk Assessment Template typically includes questions about an individual's thoughts, plans, and history of suicidal ideation or attempts, as well as their access to lethal means and protective factors.
Q: Who uses a Suicide Risk Assessment Template?
A: Mental health professionals, such as psychologists, psychiatrists, and social workers, use Suicide Risk Assessment Templates to gather information and make informed decisions about suicide risk.
Q: Why is a Suicide Risk Assessment Template important?
A: A Suicide Risk Assessment Template helps mental health professionals identify individuals who may be at risk for suicide, allowing for appropriate interventions and support to be provided.
Q: Can a Suicide Risk Assessment Template predict suicide?
A: No, a Suicide Risk Assessment Template cannot predict suicide with certainty. It is used to assess an individual's risk level and develop a safety plan, but it cannot guarantee that suicide will be prevented.